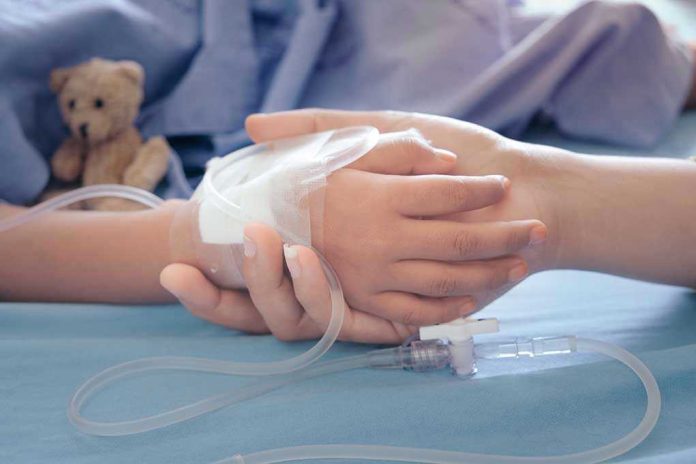
When the British state quietly rations “life‑changing” drugs for dying children behind closed‑door deals with drug companies, it exposes the gap between what the system promises and what families actually face.
Story Snapshot
- Hundreds more children with spinal muscular atrophy (SMA) are now eligible for powerful new treatments on the National Health Service after years of patient and celebrity campaigning.
- The National Institute for Health and Care Excellence (NICE) and NHS England expanded access while openly admitting long‑term evidence and safety data are still incomplete.
- Gene therapy Zolgensma and drugs like Spinraza and risdiplam can dramatically improve survival and mobility for some babies, but they carry eye‑watering price tags and strict age and eligibility rules.
- Confidential pricing deals and managed access schemes feed public suspicion that life‑and‑death decisions are shaped as much by accountants and pharmaceutical lobbyists as by doctors and parents.
What these “life‑changing” SMA drugs actually do
Spinal muscular atrophy is a rare genetic disease that destroys motor neurons, leaving babies too weak to sit, breathe, or swallow, and often killing them before age two without treatment. Zolgensma, a one‑time gene therapy, delivers a working copy of the missing gene and has been approved for National Health Service use after a deal that NHS England describes as “life‑saving.” Officials say it can help babies move and walk, potentially transforming about 80 young lives each year in England alone. [4][5]
Nusinersen, marketed as Spinraza, and risdiplam work differently, but aim at the same problem: getting the body to produce more of the survival motor neuron protein that SMA patients lack. A national agreement between NHS England, NICE, and manufacturer Biogen made Spinraza available for children, young people, and adults with SMA Types 1, 2, and 3 through a managed access scheme. That deal exists precisely so patients can receive treatment while the health service continues collecting long‑term data on whether the benefits last. [1]
How access expanded from “no options” to three powerful treatments
Only a few years ago, British clinicians had no effective medicines at all for SMA, leaving families with little more than palliative care. That changed as regulators approved Spinraza first, then Zolgensma, then risdiplam. Reporting on the latest agreement, one outlet quoted an NHS England spokesperson saying the service had “revolutionised care” by securing access to all three innovative treatments in just three years. For roughly 1,500 people with SMA in England, risdiplam alone offers a home‑based oral option instead of repeated spinal injections. [2][8]
These approvals did not arrive in a political vacuum. Families, charities, and public figures—including pop star Jesy Nelson—used media campaigns to pressure decision‑makers to move faster and widen eligibility. While the available documents do not prove that any one celebrity directly changed a vote, they show that NICE routinely hears patient and caregiver testimony when weighing ultra‑expensive drugs. In practice, emotional stories and public outrage sit alongside clinical trial tables and cost‑effectiveness models in the same cramped committee rooms. [1][2]
The price of hope: secrecy, rationing, and “fair to taxpayers” deals
Every one of these treatments comes with a staggering price tag. Press coverage has highlighted Zolgensma’s list price in the millions of pounds for a single infusion, and risdiplam at nearly £8,000 per small bottle. NHS England insists it has negotiated confidential discounts that keep prices “fair to taxpayers,” but the actual numbers and rebate formulas remain hidden from the public. That secrecy makes it impossible for outsiders to judge whether the government drove a hard bargain or folded under pressure. [2][4][8]
To square the circle between desperate parents and finite budgets, NICE and NHS England fall back on managed access agreements and strict criteria. Spinraza’s deal explicitly limits coverage while longer‑term results are gathered. For Zolgensma, NHS England later ordered a pause on funding treatment for children older than 12 months, pending safety review, even as younger babies continued to receive the gene therapy. These stop‑start rules illustrate a harsh reality: access is conditional, not guaranteed, and can be dialed back when new safety or budget concerns surface. [1][3]
Why this fight resonates beyond one rare disease
The United Kingdom’s official pathway for new medicines says patients should get timely access to drugs that are both clinically effective and cost‑effective. SMA is now a test case of how that promise plays out when treatments are genuinely transformative but also astronomically expensive. Regulators are approving medicines on the basis of small trials and short follow‑up, then trying to fill in the evidence gaps while the drugs are already in use. That approach shifts real risk onto families and taxpayers. [1][4][8]
For Americans on the left and right who already distrust “the elites,” the SMA story in Britain sounds familiar. Powerful pharmaceutical companies push sky‑high prices. Government experts insist the process is neutral and scientific, yet conduct negotiations and evidence reviews behind closed doors. Emotional campaigns by celebrities can seem to matter more than the quiet suffering of ordinary families. And even when the state finally does the right thing and funds life‑saving care, it often does so late, conditionally, and on terms the public is not allowed to see. [2][4]
Sources:
[1] Web – Life-changing SMA drug Spinraza set to be available for NHS use in …
[2] Web – Life-changing mobility drug for spinal muscular atrophy patients to …
[3] Web – Temporary change to eligibility for SMA treatment Zolgensma® in …
[4] Web – NHS England strikes deal on life-saving gene-therapy drug that can …
[5] Web – NICE approves new SMA gene therapy
[8] Web – Introducing new medicines in the NHS in the UK – pathway




